Fatal Breakthrough COVID-19 in a Heart Transplant Recipient
A 71-year-old male presented with two days’ shortness of breath, myalgias, and chills in March 2021. His temperature was 99.0 °F and heart rate was 108 beats/minute. The patient had received two doses of the COVID-19 vaccine four weeks apart, with the second dose 16 days prior to admission.
Laboratory exams were significant for lymphopenia and acute kidney injury (AKI).
His brain natriuretic peptide (BNP) level was found to be elevated (an indicator of heart failure). A chest X-ray showed cardiomegaly with pulmonary vascular engorgement and an electrocardiogram showed an atrial-sensed, ventricular-paced rhythm. 5 years prior the patient received an orthotopic heart transplant. The biopsy ruled out rejection. He also had a history of obesity, hypertension, unprovoked deep vein thrombosis, and dual chamber pacemaker.The patient was started on dexamethasone and remdesevir and his tacrolimus dose was adjusted to maintain therapeutic serum levels. The patient’s AKI improved with fluid resuscitation.
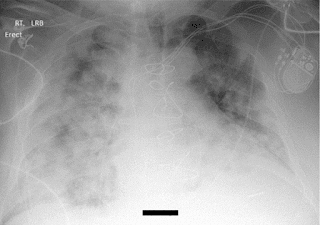
Over the course of 18 days, the patient’s respiratory status significantly worsened despite treatment with tocilizumab. Repeat chest X-rays on day 5 showed new and worsening pulmonary edema and possible multifocal pneumonia (see Figure). IgG and IgM antibodies against SARS-CoV-2 were tested and returned negative, suggesting absence of immunity against COVID-19 infection. The patient declined intubation and expired on day 18.
PS: A more recent article concluded that solid organ transplant recipients Swith suboptimal antibody responses to 4 SARS-CoV-2 doses may still benefit from a a 5th dose.
REFERENCE
Belur AD, Otero D, Dunbar Matos C. A Fatal Case of COVID-19 Pneumonia in a Fully Vaccinated Heart Transplant Recipient. The University of Louisville Journal of Respiratory Infections. 2022;6(1):13.
Comments
Post a Comment