Vaccine-induced Myocarditis and Postural Orthostatic Tachycardia Syndrome
A study published in January 2023 found that people who developed myocarditis after receiving a coronavirus vaccine had significantly higher levels of the virus's spike protein that was not bound by immune antibodies. It was also found in 10% of patients with chronic Hepatitis C up to 28 days after COVID-19 vaccination.
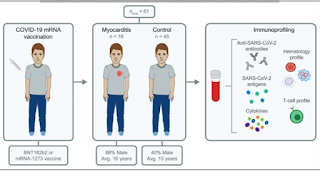
The spike protein may damage the heart's pericytes or endothelium by reducing the expression of the angiotensin-converting enzyme 2 (ACE2), reducing the production of nitric oxide in the endothelium, or activating integrin-mediated inflammation with hyperpermeability of the endothelial cell layer. The study prospectively collected blood from 16 patients with myocarditis who were hospitalized at two hospitals in Massachusetts (2 after the 1st dose, 12 after the second dose, and 2 after the 3rd dose) and compared the results to those from 45 vaccinated control subjects with no serious side effects. The individuals with myocarditis had essentially the same antibody and T-cell responses as the control subjects but had markedly higher levels of unbound spike protein and higher cytokine production. No unbound spike protein was detected in the control subjects. The authors suggest that administration of anti-spike antibodies, if spike antigen-emia is detected, could potentially prevent or reverse postvaccine myocarditis."
One of the latest published case reports about post-vaccinal myocarditis described a 13-year-old male who developed fever, headache, fatigue, and sleep disturbance on the day after receiving a second dose of the Pfizer-BioNTech COVID-19 mRNA vaccine. 2 weeks later he presented at a clinic and was treated with Acetaminophen, ibuprofen, and Chinese herbs (Goreisan and Kakkonto) but the symptoms persisted, and the patient was unable to get out of bed all day. An active standing test (AST) showed that when the patient stood, his heart rate immediately increased from 65 to 140 beats/minute (bpm). Motor nerve and sensory nerve conduction studies showed no abnormalities (see Figure). He was diagnosed with postural orthostatic tachycardia syndrome (POTS). On the 33rd day after vaccination, despite complying with the POTS regime, he was admitted to the hospital due to severe fatigue, headache, and orthostatic symptoms including lightheadedness and palpitations. Echocardiography revealed a slight pericardial effusion (3-5 mm) at the right anterior ventricle, with a 72% normal ejection fraction leading to a diagnosis of mild myocarditis.
The patient's symptoms improved after intravenous immunoglobulin for myocarditis, non-pharmacologic interventions, and multiple medications for POTS.
Another recent paper showed that in the vaccinated senior high school students, the depolarization and repolarization parameters (QRS duration and QT interval) decreased significantly after the vaccine with increasing heart rate. In total, 763 students (17.1%) had at least one cardiac symptom after the second vaccine dose, mostly chest pain and palpitations. Recent reviews highlighted the risk in males under 40 and in children and adolescents.
REFERENCES
Yonker LM, Swank Z, Bartsch YC, Burns MD, Kane A, Boribong BP, Davis JP, Loiselle M, Novak T, Senussi Y, Cheng CA, Burgess E, Edlow AG, Chou J, Dionne A, Balaguru D, Lahoud-Rahme M, Arditi M, Julg B, Randolph AG, Alter G, Fasano A, Walt DR. Circulating Spike Protein Detected in Post-COVID-19 mRNA Vaccine Myocarditis. Circulation. 2023 Jan 4. doi: 10.1161/CIRCULATIONAHA.122.061025. Epub ahead of print. PMID: 36597886.
Sanada Y, Azuma J, Hirano Y, Hasegawa Y, Yamamoto T. Overlapping Myocarditis and Postural Orthostatic Tachycardia Syndrome After COVID-19 Messenger RNA Vaccination: A Case Report. Cureus. 2022 Nov 2;14(11):e31006. doi: 10.7759/cureus.31006. PMID: 36475233; PMCID: PMC9717213.



Comments
Post a Comment