Delayed myocarditis following vaccination
A healthy 24-year-old man with a history of allergic rhinitis experienced tightness in his chest, difficulty breathing, and coughing up blood six months after exposure to COVID-19 (he never tested positive nor experienced any symptoms) and three months after a second dose of the Moderna vaccine.
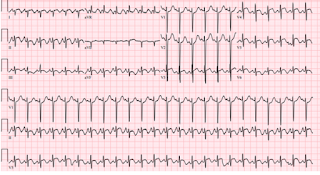
On arrival, his oxygen level was low, his heart rate was high, he had a fever, and his blood pressure was normal. He looked very sick and was sweating. Electrocardiography (ECG) showed sinus tachycardia with diffuse ST-segment elevation and T-wave inversion (Figure).
There were abnormal sounds in his lungs despite normal X-rays. His heart's electrical activity showed a fast rhythm with changes in the ST-segment and T-wave. Blood tests indicated heart damage and inflammation. An ultrasound of his heart showed that its pumping ability was reduced. A biopsy of his heart muscle confirmed inflammation Tests of fluid from his lungs showed no signs of bleeding or infection.
Diagnosis was a delayed allergic reaction to the COVID-19 vaccine. After three days of taking steroids, another ultrasound of his heart showed improved pumping function and his ECG looked better. He was sent home with a plan to gradually reduce his steroid medication and was prescribed lisinopril and carvedilol. At a follow-up appointment a month later, he said his chest tightness and difficulty breathing had improved, but he sometimes felt irregular heartbeats. A portable heart monitor showed a high number of abnormal heartbeats with temporary changes in the ST-segment and T-wave, so he had a loop recorder placed for longer-term monitoring of his heart.
REFERENCE
Janga C, Patel T, Hennawi HA, Atam S, Shah S, Naeem I, Memon R, Haas DC. Delayed presentation of biopsy-proven eosinophilic myocarditis following COVID-19 mRNA vaccine. Glob Cardiol Sci Pract. 2023 May 11;2023(2):e202310. doi: 10.21542/gcsp.2023.10. PMID: 37351099; PMCID: PMC10282781.

Comments
Post a Comment